
The emergency department (ED) can be a stressful and confusing place for individuals who are sick or injured. During the pandemic, with many hospitals not permitting friends or family to accompany ED patients, being alone may exacerbate the uncertainty, fear and anxiety patients may experience about things like waiting times, undergoing tests or medical prognoses.
Research shows that almost half of all patients leave the hospital with a poor understanding of their ED visit. As doctors who see the consequences of poor communication, let us break down what is going on in the ED and give you the knowledge and tools to empower you to have a smoother experience.
The emergency department explained
In the ED, some patients arrive by themselves (or get dropped off by family), some disembark from an ambulance and some are transferred from other hospitals. To decide the order of patient care, clinicians use a decision-making tool called the Canadian Emergency Department Triage and Acuity Scale (CTAS). The CTAS is used instead of a first-come, first-served system.
The CTAS sorts patients based on severity of the illness or injury. A score of 1 suggests an imminent risk of dying or severe disability within minutes without treatment (for example, serious car accident or stroke). A score of 5 suggests that the outcome of the medical issue will not change whether treatment is delivered now or in a few hours.
A patient’s movement around the ED, from waiting location to treatment room to investigation area, is based on the presenting illness and CTAS. Patients wait for the room with the best resources for their condition. For example, a plaster room is the best place to make a cast for a broken ankle, but does not have the heart monitor equipment for diagnosing or treating a heart attack.
These factors help explain why certain patients seem to leave the waiting room faster than others.
People in the ED
The people working in the ED include clinicians such as doctors, nurses and social workers, and non-clinical staff such as clerks, porters and housekeepers. The number and types of staff will depend on the size of hospital. Each team member has a defined role and scope of practice, resulting in a roughly predictable sequence in which patients will see each staff member.
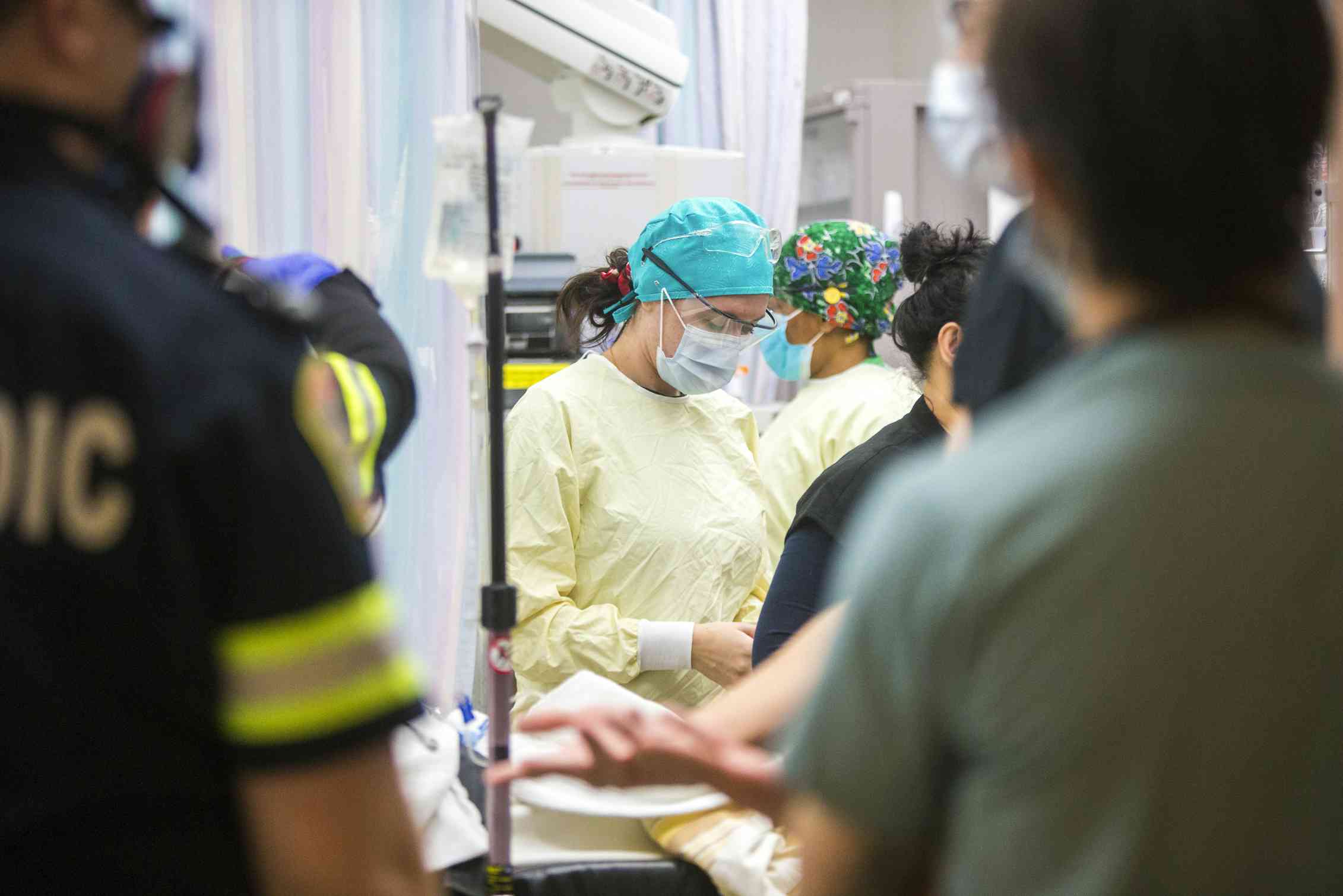
A patient entering the ED usually has their information collected by a clerk first, followed by a preliminary assessment by the triage paramedic or nurse. They may then be seen by another professional for a test or procedure like an X-ray. They may be monitored and treated by a nurse through much of this time, and seen by a physician. Before leaving the ED, a social worker or patient navigator may be seen as well.
Sometimes clinicians come and go over time, depending on whether they are waiting for results of tests or responses to treatment, so visits can differ in length. Recognizing the different roles of each employee, and different timelines, can help patients understand the process of diagnosis and treatment.
Why understanding your ED visit matters
To minimize feelings of being overwhelmed, and improve overall quality of care, patients should understand what happens in the ED. Patients may understand their diagnosis, but often have less comprehension of the followup plan. For example, approximately five to 10 per cent of patients do not fill their ED medications as prescribed and many do not follow up with recommended medical appointments.

This is partially due to a lack of understanding of their ED visit, and results in more returns to the ED and greater likelihood of hospitalization, especially for older adults.
Certain factors put patients at higher risk for leaving the ED without sufficient knowledge. These include hearing or vision challenges, cognitive impairment or altered cognition (for example, from intoxication or severe illness), speaking a primary language different than the one spoken in the ED, as well as having difficulty reading or a lack of knowledge about the health-care system or health issues.
What you can do
While the health care system needs to do its part to improve the ED experience and clearly communicate, there are evidence-based strategies that can empower patients in their own care.
- Have a list of your medications, allergies and medical conditions on hand, saved on a phone or in a wallet. It is beneficial to be as prepared as possible. Think about the questions you want to ask: What is the goal of the visit? Who will help you keep track of the recommendations? Preparing in advance can speed up the process and provide information to the health-care team.

For older people, those with mobility or sensory challenges and those who are very unwell, a family member of caregiver may call the hospital and ask to speak to a nurse or doctor to relay or receive this information if their loved one is unable to do so.
On discharge, the patient should ask for clear written instructions. Short, concise and in plain language is preferred over long medical summaries. Written is generally better than verbal instructions.
Repeat the discharge and followup instructions with the nurse or physician to check for accuracy. If the information and next steps are overwhelming, ask to speak to a discharge planning nurse or care navigator who can help smooth the transition from ED to home.
If the patient and/or loved ones see barriers to being able to follow through with a suggested care plan (such as an inability to afford medication, get to a pharmacy or swallow pills), these barriers should be brought to the ED team’s attention. It is better to address these proactively than to leave a condition under-treated.
If you are not feeling better, or are getting worse, return to the ED. Ask about return precautions: symptoms to watch for that should prompt a return to the ED. Going back may give ED staff a chance to see your symptoms at a different stage, which may result in a different course of action.
In terms of what to ask, research has shown that it’s helpful for patients to record a few important points:
- Date of ED visit and main diagnosis
- Medication details (dose, purpose and how long to take)
- Any doctors to follow up with, when and how to contact
- Symptoms that should lead to immediate return to the ED
Being knowledgeable and prepared to self-advocate can not only make the next ED visit easier and less stressful for you or your loved one, but can also help ensure you leave with the information you need.
Jasmine Mah is an Internal Medicine resident with Nova Scotia Health and receives scholarships supporting her PhD research from the Department of Medicine at Dalhousie University, Dalhousie Medical Research Foundation, Dr. Patrick Madore Foundation, Alzheimer Society of Nova Scotia and the Pierre Elliott Trudeau Foundation. She is part of the Canadian Consortium on Neurodegeneration in Aging (CCNA) Team 14, which investigates how multi-morbidity, frailty and social context modify risk of dementia and patterns of disease expression. The CCNA receives funding from the Canadian Institutes of Health Research (CNA-137794) and partner organizations (www.ccna-ccnv.ca). The affiliations/funders had no input into any aspect of this subject or article.
Melissa Andrew has received funding from Sanofi, GSK, Merck, Pfizer, Seqirus, Public Health Agency of Canada, Canadian Institutes of Health Research, and the Canadian Frailty Network, unrelated to the present article. She serves as a member of the Alzheimer Society of Nova Scotia Board of Directors and is part of the Canadian Consortium on Neurodegeneration in Aging (CCNA) Team 14, which investigates how multi-morbidity, frailty and social context modify risk of dementia and patterns of disease expression. The CCNA receives funding from the Canadian Institutes of Health Research (CNA-137794) and partner organizations (www.ccna-ccnv.ca).
